DISCOVER THE SHOULDICE DIFFERENCE. More than 98% of our cases are performed with our natural tissue technique...without the use of mesh.
The Shouldice success rate for hernia repair sets the gold standard for medical professionals around the world. Clinical evidence, gathered over 75 years of follow-up with our patients, clearly demonstrates that the hernia repairs performed at Shouldice Hospital are exceptionally safe, secure, and reliable. Although there are inherent risks in any surgery, there are no similar or comparable risks in natural tissue hernia repair versus mesh. Scar tissue of natural tissue left in a place represents no risk, while mesh left behind can continue its erosion and potential migration within the body.
Mesh should never be used because it’s easier, faster, cheaper, or due to a lack of familiarity with, or expertise in, the use of natural-tissue techniques!
The most common types of hernias develop within the abdominal wall which runs from the rib cage down to the groin. It is the strong wall of muscle and tissue that holds your organs (such as your stomach and intestines) inside the abdomen.
When tissues or organs bulge through a weakness in your abdominal wall, it is called a “hernia”. A hernia repair is simply reducing the content of the hernia sac (returning the protruding organs back into the abdominal cavity) and repairing the weakness in the abdominal wall.
There are many types of abdominal wall hernias and they are usually classified based on their anatomical location. The most common hernias are fully explained, and graphically detailed, in the videos below, and can be classified as follows:
Groin Hernias
The groin is the area just above the skin crease, where the upper leg meets the abdomen and up to a line from hip bone to hip bone. The lower area of the groin is the weakest part of the abdominal wall, and is the area where hernias most often develop.
There are two types of groin hernias:
Inguinal hernias appear in the groin or scrotum and are subdivided into direct (directly through the abdominal wall) and indirect (down the inguinal canal); and
Femoral hernias appear in the lower part of the groin or upper thigh.
Ventral Hernias appear in the abdominal wall (usually above the groin area) and can occur through a previous operation’s incision site (incisional), around the navel (umbilical), above the navel (epigastric), or at any other weak muscle site (primary abdominal).
Hernias are usually divided into two main categories:
Congenital
Congenital hernias develop before you are born and are present at birth, and may not be diagnosed for weeks, months or even years. A hernia that develops much later in life may actually result from a weakness that you have had since you were a baby. In boys, the weakness results from the failure of the sac that precedes the testicle during its decent through the abdominal wall down the inguinal canal into the scrotum to close. In girls, the weakness is caused by a similar failure of the opening that allows the round ligament of the uterus to pass through the inguinal canal to close.
In fact, inguinal hernias occur in up to 5% of full-term and 30% pre-term infants, and are often seen by mothers who notice a bulge in their baby’s lower groin when they cry.
Acquired
Acquired hernias develop when the muscles, or connective tissue, in your abdomen are weakened or damaged during your lifetime, and the body’s natural cycle of tissue breakdown and repair is disrupted. This can be due to aging, or a poor balancing of replacement good versus bad collagen tissue, the building block of all wounds. Although this explanation sounds very simple, hernias are actually quite complex.
Incisional hernias can develop in up to 50% of patients who have had prior open abdominal operations, and can also occur in port sites used in laparoscopic surgery (trocar hernias).
Some patients have congenital conditions that interrupt the body’s natural healing processes, while others negatively affect healing through their lifestyle choices; for example, smoking.
What causes muscles to weaken?
Your body is constantly involved in a well-balanced equilibrium between old tissue breakdown and new tissue replacement. As you age, the enzymes that help to control this natural process can get out of balance. When your body cannot balance the build and repair cycle, weak spots may develop in your ligaments and connective tissues, particularly noticeable in the groin area. Over time, your tissues may also be weakened by other factors, including poor nutrition, diabetes, smoking, obesity / excessive weight gain, injuries and surgical operations.
The most common sign of a hernia is a soft swelling or bulge under your skin. The type of hernia you have will determine where the bulge appears on your body. Some hernias can only be seen when you stand up, and may disappear completely when you lie down. Others may only be visible when you strain your muscles by coughing, sneezing, laughing, bending or lifting. Usually, the bulge is soft enough that you can gently push, or knead, it back into your abdomen (reducible), and it is often not there when you wake up in the morning.
Most hernias are not painful. However, sometimes the area around your hernia may be tender and you may feel some sharp twinges or a pulling sensation. As your hernia gets bigger, your pain and discomfort may increase. If not repaired, a hernia may eventually prevent you from enjoying normal activities due to increased discomfort, such as exercising, working, household chores or sex.
Health Risks
When an organ, such as your intestine (bowel), pushes through the abdominal wall, there is a small risk it could become trapped. This is known as an incarcerated hernia. If your hernia is trapped outside of the abdominal wall, you won‘t be able to push it back into your abdomen, and it may feel hard and be very painful. Contact your doctor right away if you have this situation.
If left untreated, an incarcerated hernia may become strangulated. This means the hernia is tightly trapped and blood will no longer flow into the tissues. Without a normal blood supply, the trapped tissues may die. A strangulated hernia is not very common and will cause severe pain, nausea, vomiting and even death. A strangulated hernia requires immediate surgical attention at the nearest hospital. Leaving a hernia until this stage means that you will lose the option of choosing the ideal type of repair for the hernia you may have.
If you have a hernia, contact your doctor right away if:
- your hernia becomes painful,
- your hernia can‘t be pushed back into your abdomen, and
- you feel sick to your stomach or vomit, have a fever, diarrhea, cannot pass gas or have a bowel movement
Hernia or groin strain?
It‘s not always easy to diagnose a hernia and there are a dozen things that can cause pain in the groin. Every year, over 1,000 patients come to the Shouldice Hospital convinced they have a hernia, when, in fact, what they really have is a groin strain. Surgery is not the right solution for these patients.
If you think you might have a hernia, please come to the Shouldice Hospital walk-in clinic for an examination. Our highly specialized surgeons diagnose and treat thousands of hernias every year. We have the expertise to provide a proper diagnosis and may help you avoid an unnecessary operation. Examinations in our walk-in clinic are provided at no cost to our patients.
Are you at risk?
Anyone can develop a hernia – it does not matter whether you are male or female, young or old, physically active or inactive. But you may be at higher risk if you:
- Are male – men have a natural weakness in the groin area that increases their hernia risk;
- Are over age 35 – as we age, our tissues naturally become weaker;
- Are born with a hereditary condition which causes poor muscles, ligaments or connective tissues;
- Have close family relatives with hernias – weakness in tissues may run in families;
- Lift heavier objects – this may reveal or aggravate existing tissue weaknesses;
- Are overweight or obese – carrying extra weight may stretch or weaken your abdominal wall, particularly at previous incision sites;
- Have a heavy or chronic cough – the force of a cough or sneeze can tear weakened muscles and connective tissue;
- Are frequently constipated – straining to have a bowel movement puts pressure on the muscles and connective tissue in your abdomen;
- Have a sports injury or accident that tears the muscles or connective tissue in your abdomen; or
- Are a smoker – smoking adversely affects the body’s ability to produce good collagen which helps promote healthy cell creation and growth of connective tissue.
Hernias can, on occasions, be difficult to diagnose. They can be present and then disappear. When this happens, the hernia does not repair itself, rather, the hernia defect, or hernia sac, simply goes back inside your abdomen through the same weakness in the abdominal wall - the weakness however, remains until it is surgically repaired.
Hernias may be identified by Ultrasound, CT scan or MRI (all of which are rarely needed) but the most reliable way is by a physical exam by a surgeon experienced in hernia repair. Diagnostic imaging “may” show that there are protrusions in the abdominal wall, but they cannot always differentiate the size of the actual hernia defect, or, whether the protrusion is a hernia versus a natural fold of the abdominal wall. Shouldice surgeons see hundreds of patients a year where initial diagnosis based on imaging confirmed the existence of a hernia, when in fact no hernia was clinically present. In these cases it may be better to wait and see if an actual hernia presents itself rather committing to unnecessary surgery.
As well, the absence of a hernia on a diagnostic image does not in itself mean there is no hernia, as surgeons at Shouldice encounter cases where imaging was negative for a hernia when, in fact, a hernia was present on examination.
Hernias will not get better by themselves. If you have a hernia, you will probably need an operation to repair the weak spot in your abdominal wall at some point. A hernia that is not repaired can get bigger, and may lead to more serious health problems. In fact, 70 to 80% of patients that have been diagnosed with a hernia have surgery within 6 years due to the ongoing risk of complications and discomfort. This is particularly true for femoral hernias, which have a much higher risk of developing complications – surgery is recommended for all femoral hernias as soon as possible.
In some cases however, a hernia may be diagnosed but that does not mean it has to be repaired right away. For example, an ultrasound may identify a hernia at a very early stage, when it is still quite small. Your doctor may suggest a period of “watchful waiting” to see how the hernia develops. If it stays small and does not interfere with your health or quality of life, an operation may not be necessary. An experienced hernia surgeon will be able to make an accurate diagnosis, and recommend a treatment plan, in this type of situation.
The type of hernia repair performed by your surgeon will depend on the size and location of the hernia, anaesthesia risk, strength of the surrounding tissue and the expertise of the Surgeon.
Hernias can be repaired in one of the following two ways:
- Using your Natural Tissue without the use of surgical mesh. These repairs are often called “anatomical” repairs as they use your own tissue to repair the hernia defect.
Natural tissue repairs are always performed using an “open anterior” surgical procedure which entails making an open incision over the hernia site, in contrast to laparoscopic procedures as outlined below.
Groin hernias make up over 80% of all abdominal wall hernias, and over the past 100 years, many natural tissue repairs have been developed with the Bassini, McVay and Shouldice methods being the most recognized. Although all these methods differ in their approach to reconstructing the abdominal wall, they are all similar in that they use the body’s natural tissue instead of mesh, and use permanent sutures to approximate the surrounding tissue around the hernia defect and repair the posterior wall of the inguinal canal.
Natural tissue repairs can be used to successfully repair virtually all direct and in-direct inguinal hernias and many ventral hernias. Mesh is most often required when the surrounding natural tissue is inadequate, or of poor quality, to allow for a strong anatomical repair – this is most often seen when repairing femoral, large incisional and recurrent hernias. Shouldice Hospital uses natural tissue repair whenever possible, or in over 98% of all its hernia cases.
Natural tissue repairs can safely be done using local and conscious IV sedation which avoids the complications of general anaesthesia.
2. Using Synthetic Mesh to either “patch” or “plug” the hernia defect instead of your natural tissue. Hernia repair using mesh can be done by using either the “open anterior” surgical technique or using a Laparoscopic approach.
a) Open anterior mesh repairs use the same initial approach as natural tissue repairs, however, instead of suturing the fascial tissue and muscle layers together to repair the hernia defect, synthetic mesh is used. There are many types of mesh repair techniques but the most recognized is the Lichtenstein patch technique (75% of all cases), plus numerous others which includes Plugs, Plugs and Patches and other hybrid systems.
In the patch method (Lichtenstien) the hernia defect is overlaid with synthetic mesh which is then secured using either sutures or with a range of other methods including tacks, staples or glues.
In the plug method (Rutkow), a mesh plug is used to fill the hernia defect like a cork stoppering a bottle. The plug is then secured by a variety of methods.
In plug and patch systems, an overlay mesh patch is anchored over the plug. In other hybrid techniques an underlaid patch is added to the overlaid patch and plug to form a once piece plug with top and bottom mesh patches. The underlaid patch is “splayed” and left unsecured while the overlaid patch is anchored.
What is common in all these techniques is the anchoring of the mesh, which puts tension on the surrounding tissues, particularly over time as the mesh shrinks and hardens.
Some of these methods often claim they are not anchored (tension free, at least initially) but this in itself creates issues when the mesh moves or “migrates”. These are more fully outlined in the section natural tissue vs. mesh in hernia repair.
b) Laparoscopic repairs are always performed under General Anaesthetic and always use mesh, as it is very difficult to do a true anatomical or natural tissue repair laparoscopically.
In this approach, three 1 cm punctures are made in the abdominal wall, one to allow a surgical scope to be inserted, along with two additional narrow tubes (trocars) to allow placement of the surgical instruments. The abdomen is inflated with carbon dioxide to create a positive pressure in the abdominal cavity that allows the bowel to fall away from the operative site, thus identifying the hernia. The hernia is then repaired by stapling, tacking or glueing a mesh patch over the defect from behind (“posterior”).
Laparoscopic techniques require the use of general anaesthesia which in itself has its own well recognized risks. Although this method is marketed by those who use it as “minimally invasive”, in reality, it is more invasive than “open” techniques as it involves penetration of the abdominal cavity. It is well recognized that Laparoscopic methods have their own associated risks, which include intra-operative complications arising from damaging internal organs during surgery, bleeding as well as leaving trochar incision scars, that in turn can become incisional hernias (fatalities have been recorded in rare circumstances).
In addition, laparoscopy is expensive and is difficult to perform. Experts have indicated that it can take doing over 600 repetitive procedures to master the technique, and few surgeons have that level of experience repairing hernias using this technique. Although laparoscopy is successfully used in many surgical areas (for example, gall bladder) it is estimated that after 25 years from its introduction that only 10-15% of hernia surgery is done laparoscopically, and many surgeons are abandoning the procedure.
The New England Journal of Medicine concluded in 2004 that “the open technique is superior to the laparoscopic technique for mesh repair of primary hernias.” (NTD – link to Article). In that article, recurrence rates for primary hernia repair, using laparoscopic techniques, were over 2 times higher than when an open technique was used. Related post-operative complications were also higher in the laparoscopic group. It is fair to note, regarding both techniques, that these results would vary in the hands of surgeons specializing in hernia surgery.
Open repairs have been associated with slightly more pain immediately after surgery and producing unsightly scarring. However, this pain, if any, quickly subsides, and when performed by an experienced surgeon, open repairs leave little, to no, permanent scarring.
Today, much is being made of new “robotic” techniques. None of these have been proven to be better than the skilled hands of an experienced surgeon, all remain extremely expensive, and all come with the same associated risks of traditional laparoscopy.
At all times the human body tolerates its own natural tissues best, and hernia surgery is no exception.
The abdominal wall is a complex multi-levelled structure made up of distinct layers of muscle and fascia (tissue) designed to contract, stretch and bear tension in a way that allows the torso to bend and twist. Anything that restricts or interferes with the normal abdominal movement puts unnatural, and often harmful, stress on the area.
For over 100 years, non-mesh hernia repairs were the gold standard in hernia repair. From Bassini’s pioneering work in the 1880’s, through natural-tissue’s evolution by McVay and E.E. Shouldice, recurrence rates of hernia specialty surgeons improved to less than 1%, and complications and long term post-operative pain were virtually non-existent at less than 1%. The problem was that not all surgeons learned how to do natural-tissue repairs correctly, and recurrence rates were highly variable, with some as high as 20% and even 40%!
In response to these inconsistent results, the surgical community looked for a way to reduce recurrences for all surgeons. Although mesh made of a wide range of materials (silver, tantalum, kangaroo tendons etc.) had been experimented with as early as 1900, it was not until the production of synthetic meshes through the 1940’s and 50’s to include polypropylene, that mesh seemed to have become truly viable in hernia repair. In the early 1990’s, after extensive promotion by mesh manufacturers, and various surgeons citing low recurrence rates and ease of surgery, mesh grew to become the standard of care. The problem was that no one knew what the risks were as no one had studied the long-term impacts of implanted mesh.
The benefits and risks of the use of mesh in hernia repair is one of the most hotly contested topics in surgery today. Ground breaking research using the latest magnification technologies is currently being carried out to explore the complicated interactions of mesh within the human body, but through conventional research and observation we have become more informed on the relative merits and risks of using mesh in hernia repair. The literature is extensive, and is often contradictory, as commercial and self-serving interests combat science and objective research; however, the following is now generally held true:
- After 120 years of natural-tissue repair, and 30 years of established mesh repairs (25 years using of laparoscopy), all techniques are roughly equivalent in terms of hernia recurrence when performed by surgeons not specializing in hernia surgery. The advent of mesh has succeeded in reducing the overall recurrence rate by surgeons who on average do 50 cases or less a year, and who are not necessarily hernia specialists, to approximately 5%. Surgeons who specialize in high volume hernia repair produce consistently better results.
- Despite the improvement in the overall recurrence rate due to mesh in the hands of non-hernia specialists, it appears to have come at a needless cost to patients. Hernia centres specializing in natural-tissue inguinal hernia repair have met, and far exceeded, 5% recurrence rates, and Shouldice has done so for over 70 years. Although it is fair to conclude that mesh has reduced overall recurrence rates, the same result could have been achieved, or bettered, by continuing to use known and proven natural-tissue techniques in specialized hernia centres without the unintended post-operative consequences now attributed to the use of mesh, as outlined below.
- The known complications of using mesh are potentially significant, and are mostly attributable to:
- Foreign body reaction – mesh is a foreign substance and your body is constantly trying to defend itself by getting rid of it;
- Movement of the mesh - despite being anchored (stapled, glued or tacked) mesh can become loose and move, or migrate, throughout your groin or abdominal cavity. It can also fold, or be caused to move, as your body tries to eject the foreign mesh body;
- Mesh shrinkage – mesh repairs depend on scar tissue to grow into the mesh, forming a large layer of scar tissue. As the scar tissue shrinks, so does the mesh, creating a hard, fibrous mass with nerves embedded within it; and
- The nature of the mesh material – all mesh, regardless of weight or thickness, has fibres that create a lattice of holes or pores. During the normal healing process nerves regenerate and grow and can be trapped within the lattice structure. Over time, the mesh also hardens and become less flexible to the point where explanted mesh samples have become hardened plastic. Mesh can also adhere to surrounding tissue, nerves and organs. This is particularly true for mesh inserted laparoscopically. To combat this risk, mesh manufacturers added protective coatings on the mesh and developed absorbable and biological mesh. All these efforts have failed. Coatings dissolve, leaving the same polypropylene to cause its complications, with absorbable mesh ending in hernia recurrence in virtually all cases, as the mesh reinforcement deteriorates during its absorption.
These factors can cause the following devastating events:
- Chronic pain (arising or lasting more than 3 to 6 months from surgery) – the incidence of chronic post-herniorrhaphy pain in published literature is highly varied due to the inherent difficulties in defining and reporting individual’s pain levels. However, most studies agree that pain severe enough to bring a change in lifestyle, to cause a severe handicap in ordinary activities, or make life unbearable, is between 12% to 15% (some estimates are as high as 60%). The reality is that mesh does not have to be placed in the wrong place, or to function incorrectly, to cause pain. It is impossible for any surgeon when placing mesh to avoid contact with all nerves – this inherent limitation with mesh can produce pain through:
- Nerve entrapment or ingrowth in the mesh lattice – think of ivy as your nerves, growing through a screen door, and having the screen shrink up to 40% in the first 5 years and eventually to become a hard mass;
- Mesh fibres eroding over time and penetrating intestines, bladder, vas deferens or other vascular structures; and
- Chronic inflammation of tissues caused by the foreign body reaction and scarring.
- Dysejaculation (excruciating and searing pain during ejaculation), Sexual pain and orchialgia (long-term pain of the testes) as a result of movement or migration of mesh penetrating the layers of the spermatic cord and the vas deferens. In extreme cases, mesh can actually invade the entire spermatic cord causing pain. Infertility can also be a problem in bilateral inguinal hernias, and the results may not be seen for 7-12 years. These effects of mesh are irreversible. Since the general adoption of mesh in the 1990’s, the incidence of Dysejaculation has risen to 3.1%, a 7,750% increase from when natural-tissue repairs were the standard of care.
- Severe Infection – many of the coatings designed to protect the mesh have in themselves caused life threatening infections;
- Hernia recurrence – to be effective the abdominal wall must remain flexible as the torso twists and rotates. As mesh hardens, it becomes more rigid and has little tensile strength. This can cause the hernia repair to fail. In addition, absorbable and biological meshes, designed to minimize scarring and foreign body reactions, when used independently, have little long-term value. Recurrence rates have approached 100% for these products; and
- Complicated surgery to remove the mesh – mesh cannot be removed like peeling off a sticky note. Over time, it becomes embedded in the surrounding tissues and organs, and its removal can involve risky surgery with uncertain results and consequences.
Although there are inherent risks in any surgery, there are no similar or comparable risks in natural tissue hernia repair, where mesh has to be peeled off a bladder, colon, a spermatic cord or a major blood vessel. Scar tissue of natural tissue left in place represents no risk, while mesh left behind can continue its erosion and potential migration within the body.
So, after all the above does mesh have a place in hernia surgery? The fair answer is “yes”.
All surgeons strive for the best surgical outcome, and there are times when the patient’s underlying tissue is so weak, damaged or non-existent that their natural tissue cannot support the hernia repair without mesh reinforcement. In these cases mesh can be an alternative.
However, this decision must be based on surgical necessity, and then, only after a thorough examination of the patient’s underlying tissue, and full assessment of the risks and benefits of using mesh. Mesh should never be used because it’s easier, faster, cheaper or due to lack of familiarity with, or expertise in, the use of natural-tissue techniques!
For over 70 years, Shouldice Hospital has been committed to repairing hernias whenever possible using your own natural tissue, and we do so in over 98% of all cases.
Why introduce a foreign body that ignores physiology, and does not match human tissue and anatomy, where natural-tissue techniques can successfully and safely repair the hernia and restore the body’s natural anatomy?
Few people know that Shouldice Hospital was a pioneer in the early development of mesh in the 1980’s. We are not “anti-mesh”; rather, “we are against the indiscriminate and injudicious use of mesh”.
Why do we avoid the use of mesh whenever possible? The answer is simple. “No mesh technique has surpassed the results achieved by the experienced surgeons of Shouldice Hospital when natural tissue repairs are used to repair the hernia defect”.
Our recurrence rate for primary inguinal hernias of around 1% is more than comparable to the best results of any mesh surgeon in the world, yet we do so with a complication rate of <0.005 (less than one half of one percent). When we compare this with the growing evidence of mesh related complications ranging between 10 and 20% it is hard to justify the use of mesh when there are safer, and more reliable, natural tissue alternatives.
The obvious question is why do we use mesh at all? The answer is again simple. To achieve the best surgical outcome, not all hernias can be repaired using the body’s natural tissue. There are times when the tissues surrounding the hernia defect are so poor, damaged or missing, that mesh must be used to reinforce the repair. Mesh, at times, may be required when repairing recurrent hernias, incisional hernias, most femoral hernias and large umbilical hernias. Mesh is rarely required in any primary direct inguinal hernia, and virtually never needed for primary indirect inguinal hernia repair.
Almost all of the hernia repairs at Shouldice are done using local and IV conscious sedation which enables patients to sleep during the operation and adds to the safety of our technique. This approach improves recovery, and ensures that our patients are comfortable during surgery. Additional medication may be used when necessary or, in some rare cases, a general anaesthetic may be required.
Most importantly, while working at Shouldice, every surgeon on the Shouldice team focuses their professional time and training on becoming an expert on the successful lifelong repair of external abdominal wall hernias. On average, each Shouldice surgeon performs over 700 hernia operations a year, giving them the experience, and skills, to expertly manage even the most complex hernia repair. When it comes to successful hernia repairs, there is simply no substitute for repetition and experience.
In a [Can J Surg, Vol.59, No.1, February 2016] landmark study, originating independently of Shouldice, from the University of Toronto 1 (NTR – link to Article) 235,192 hernia patients were followed-up over a 14 year period (1993-2007) with a total follow-up period of 16 years and 3 months. All patients had primary groin repairs, and were divided into 5 populations based on the volume of hernias performed at the respective hospital. Shouldice patients represented one entire group for direct comparison. The published results revealed that the recurrence rate of all general hospitals in the Province of Ontario ranged from 5.21% among lowest volume hospitals to 4.79% for patients at the highest volume hospitals. By contrast patients who had surgery at Shouldice Hospital had standardized recurrence risk of 1.15%. Within these populations mesh was used in 85.7% of patients in non-Shouldice hospitals and in only 1.46% at the Shouldice Hospital.
The Operation
The muscles and connective tissue of the abdominal wall are arranged in three separate layers. Before repairing any weakness, we gently place fatty tissue, and any part of the intestine (bowel) that may have bulged through the abdominal wall, back inside the abdomen. Then we repair each muscle layer individually, using a technique that puts virtually no immediate, nor long-term, tension on the natural tissue. By carefully overlapping and securing each layer, just like you do when you button a coat, we strengthen and reinforce this section of the abdominal wall using only your natural tissue.
As part of the Shouldice procedure, we do a thorough search for other hernias, or weaknesses, in the area and repair them as well. This aspect of our technique is unique and not commonly practiced elsewhere, as most natural-tissue techniques (including Desarda), or virtually all open mesh techniques, do not go deep enough into the pre-peritoneal space to allow exploration of the whole area. Research has shown that up to 13% of people with hernias have a second weak spot in their muscles, or a "hidden" hernia. Our skilled surgeons have the expertise to find these hidden threats; in fact, it‘s one of the most important benefits of the Shouldice repair, by avoiding the need for a potential second surgery.
At Shouldice, we firmly believe that it is in the best interests of our patients to cure hernias permanently by finding and repairing all secondary hernias the first time.
The Recovery
Patient recovery begins the moment the operation is over. Patients not requiring general anaesthesia are able to walk out of the operating room, assisted by the surgical team to a wheelchair, and comfortably returned to their room. Within hours patients will be up and about, and by the next morning, doing gentle exercises along with all the other patients. Throughout their stay patients are supported by a buddy system, their roommate and new friends, who are sharing the same experience. This allows for discussion and comparison of their recovery, thus alleviating anxiety and stress that would be taken home to their family.
During the recovery, patients receive a holistic program of patient care that encourages a safe, healthy and rapid return to normal activities. Most of our patients are back to their regular routines in less than a week, and some even go back to work as soon as they are discharged from the hospital.
Our repair techniques have been widely acclaimed, but it is the total Shouldice experience that underlies our success and attracts patients from around the world to our hospital.
The term “Tension-Free”, as applied to hernia repair, is a concept invented by competing hernia repair techniques (both natural-tissue and surgical mesh) to try and differentiate themselves by implying that “tension” is bad, and that their technique is better, because their repair did not introduce tension on the underlying tissue surrounding the repaired hernia defect.
The reality is that tension is not the enemy of hernia repair as it exists naturally throughout the abdominal wall. All hernia repairs by their nature involve realigning tension within the abdominal wall by repairing the tear or weakness in the muscle. The key is what happens to that tension over time.
Natural tissue techniques can put immediate, but minimal, tension on the muscles and surrounding tissues as they are drawn to repair the hernia, but this mild discomfort subsides quickly as the tissues stretch and compensate in the natural healing process through muscular adaptation so well described by physiologists and seen in weight lifters. Thereafter, only the strengthened natural tissue abdominal wall remains.
With mesh techniques, the issue is that mesh cannot match the properties of natural tissue, and this inconsistency of tension, over time, puts mechanical stress and undue long-term tension on the mesh which will shrink, crack, harden and may become displaced while dragging new entrapped nerves within its pores.
There are 100’s of research papers that conclude that mesh shrinks significantly over time, and it is generally recognized that after 5 years implanted mesh will shrink up to 40%, lose the majority of its pliability and eventually turn hard into a solid mass. This can be seen in the image below of a piece of virgin mesh, prior to it being implanted, compared to a piece of extracted mesh.

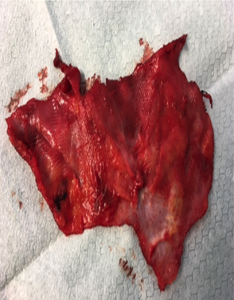
Pain after hernia surgery usually subsides within 2 weeks, and persistence after 3 months is considered abnormal. After 3 to 6 months, if the pain is still present, it is referred to as chronic post-operative pain.
The incidence of chronic pain after hernia surgery with mesh is highly debated. Rates ranging from 0% to 60% have been widely reported, but a general consensus within the expert hernia surgical community, a reliable incidence of 12% to 15% is recognized.
Traditional approaches of pain management such as pain and nerve medication, nerve blocks or nerve removal or dissection do not last long, nor are they effective in the long run, as they are intended to only block the pain, and do not treat the cause of the pain.
To date, the only potential permanent solution to this chronic pain issue is to have the mesh removed.
The removal of surgical mesh can be difficult. The success in reducing associated pain and discomfort is dependent on many factors such as: where the mesh was originally laid, the size of the mesh, the type of mesh, the extent of the inflammatory reaction and of the mesh’s migration within the body over time, how long the mesh has been inside your body, and the degree of invasion of nerves and organs which have become adherent to the mesh thus initiating erosion into the adjacent tissues. All these factors dictate how much of the mesh can be safely removed, and how much relief can be obtained.
The removal of mesh after hernia repair is a relatively new procedure, and accurate figures on its success are still being compiled as patients who have had the procedure are being followed and assessed. However, preliminary indications are encouraging, where early reports have confirmed a level of pain reduction in over 90% of cases after the mesh was removed. Levels of improvement varied widely, from slightly better to a total cure. In some cases the pain remained unchanged (5%), while in a lesser group (2%), the pain actually became worse. Early experience believes that these unfortunate cases are due to the impossibility of removing the entire mesh, which may have become too adherent, penetrated major blood vessels or infiltrated organs.
Mesh removal should only be attempted by surgeons specialized in this procedure, and patients should be realistic with respect to the possible success of this treatment for their pain.
The best decision is not to have surgical mesh implanted in the first place.
The decision as to who should repair your hernia is critical to your surgical outcome, and it is dependent on what can be an overwhelming experience. To help you through that process, here are the key issues you should discuss with your surgeon:
- Is surgery necessary now, or is watchful waiting a better alternative? Get a complete understanding of the risks of waiting to have your hernia repaired;
- How many hernia repairs have they performed, and are they fluent with all the current medical literature surrounding hernia treatment options, repair techniques and complications associated with the use of mesh? Ensure your surgeon specializes in hernia repair, as there is no substitute for training and experience. All studies confirm that surgical outcomes improve with surgical repetition and volume. This is especially true, and critical, when it comes to surgeons who use the Laparoscopic approach;
- What kind of hernia repair do they plan to perform, and why? Your surgeon should be able to outline all the surgical alternatives and the benefits and risks associated with each. In particular, ask about the use of mesh, and why a natural tissue alternative is not appropriate;
- What are their rates of hernia recurrence, post-operative complications and risk of chronic pain? Surgeons should know these, and the good ones are willing to discuss their results. Be sure to ask how long they track their patients, as your hernia repair should last a lifetime;
- What are their hospital’s infection rates? Hospital / facility acquired infections can be serious, and your surgeon should strive to minimize these risks whenever possible.
- Is their Hospital / facility appropriately licensed, do they follow best practices, and is their operating room staff fully qualified and trained? All these factors can have an important impact on the success of your surgery; and
- What level of post-operative support can you expect from both your surgeon and the hospital / facility staff? Although post-operative complications are rare they can happen, and you should ensure you have adequate access to care and support after your surgery. In particular, ask, if mesh is to be used, what is the prognosis if you experience chronic pain?
At the end of your consultation, make sure you have had all your questions fully answered before you commit to surgery. If you do not have absolute confidence in your decision, get a second opinion.
After careful consideration of the factors above, we are confident that you will entrust Shouldice Hospital and its experienced team of surgeons, nurses and support staff to perform your hernia surgery and post-operative care.
When you are overweight, fat not only collects in a layer between your skin and underlying tissues but it can also increase the fat content within muscle tissue. Because fat is very soft, the muscle fibres of the abdominal wall become weaker.
It has been our experience that achieving a healthy weight contributes to the long-term success of your hernia repair by improving the muscle tissue used to repair the hernia defect – this is especially true for incisional and umbilical hernias. It also makes it easier for your surgeon to reach and repair the hernia, as well as improving the effectiveness of local anaesthetic, making for a more comfortable operation.
We know that losing weight can be a difficult task, especially if your hernia is limiting your ability to exercise. We have a Registered Dietitian on staff to provide expert guidance in developing specialized weight loss programs, to help you make healthy choices for long-term weight maintenance, and to follow up with you to encourage you and to monitor your progress.
This advice can include our time-tested Shouldice Diet that has helped thousands of patients achieve their weight loss targets. Not all weight loss improves muscle tissue – our diet is designed specifically to help patients lose weight (fat) quickly and safely, and to do so in a way that contributes to the success of your hernia repair.
An important lifestyle change.
Many of our patients have benefited so much from their weight loss program that they have made a long-term commitment to maintaining a healthier weight to improve their quality of life. Getting your body in shape for your hernia repair may be just the motivation you need to change your lifestyle for the better. We know you can do it, and we‘re there to help if you need it!
THE MOST COMMON TYPES OF EXTERNAL ABDOMINAL WALL HERNIAS
This is the most common type of hernia, representing 60% of all external abdominal wall hernias. Men have a much higher risk of developing an indirect inguinal hernia than women. That is because, before they are born, men have a natural opening in their groin, where the spermatic cord and the testicles pass out of the abdomen into the scrotum. The path that the testicles travel into the scrotum is called the inguinal canal.
Sometimes, the opening at the top of the inguinal canal does not close properly after the testicles have passed through. The opening weakens the abdominal wall, increasing the risk that a hernia may develop. This is called a congenital weakness because it is usually present when you are born. Women also have an inguinal canal but they are far less likely to develop a weak spot in this area because they do not have a spermatic cord passing out of the abdomen.
If you have an indirect inguinal hernia, it means that fat or, part of your intestine (also called the bowel) has slipped through a weak spot in your abdominal wall. The hernia may appear as a small bulge on one or both sides of your groin. If it is not repaired, an indirect inguinal hernia will almost always get larger, as more fat or tissue bulges through the abdominal wall. In men, the hernia may gradually move right down the inguinal canal into the scrotum.
Femoral hernias are rare. They are more common in women who have been pregnant or are obese but they can also occur in men. A femoral hernia develops when fat or part of your intestine (also called the bowel) pushes through a weak spot in the muscles or tissue and enters the femoral canal. The femoral canal is a passageway that carries large blood vessels in and out of your leg.
This type of hernia will appear as a small bulge at the groin crease just above your thigh and may be misdiagnosed as an inguinal hernia. As it gets larger, it will move down into your leg. If you have a femoral hernia, there is a greater (but still small) risk that part of your intestine may get trapped. This is called an “incarcerated hernia” and can lead to a life-threatening emergency known as a strangulated hernia. The risk of strangulation is higher in femoral hernias.
Learn to recognize the symptoms of a trapped hernia.
Direct inguinal hernias occur most often in men but may also affect women. This type of hernia may develop when the body’s continuous cycle of breaking down and building up tissue is no longer in balance, causing weak spots to develop in the muscles and tissue. Increased pressure or straining can also weaken the muscles or connective tissue of the abdomen. Increased pressure can be caused by weight gain, sports injuries or activities such as heavy lifting, chronic coughing, vomiting or straining on the toilet due to constipation. Learn more about the causes of hernias.
If you have a direct inguinal hernia, it means that fat or, in rare cases, part of your intestine (also called the bowel) has slipped through a weak spot in the abdominal wall. Direct inguinal hernias may get bigger over time but do not usually get large enough to reach the scrotum.
Epigastric hernias can develop in both women and men. This type of hernia appears as a bulge in the area below the ribcage and above the belly button. At first, the bulge may be small but epigastric hernias can become quite large over time.
Epigastric hernias usually develop in people who are born with a weak spot in their abdominal muscles. If you have this type of weakness, any forceful activity, such as sneezing, coughing or lifting heavy objects, could be all it takes to push abdominal fat through the opening.
An umbilical hernia develops in the area of your belly button. This type of hernia is seen most often in babies and young children. It can also develop in pregnant women and in people who are overweight or obese.
An incisional hernia is caused by weakening in the scar tissue that develops after you have had an operation on your abdomen. If you gain a lot of weight after an operation, you are at higher risk of developing an incisional hernia. Forceful activities, such as coughing, sneezing or lifting heavy weights, may also lead to this type of hernia.
-
SHOULDICE HOSPITAL ADDRESS
7750 Bayview Avenue,
Thornhill, Ontario,
Canada L3T 4A3
View Map -
CONTACT US
Tel: 905-889-1125
Fax: 905-889-4216
Canada: 1-800-291-7750
U.S./International: 1-855-328-3423
postoffice@shouldice.com -
ACCESSIBILITY
Shouldice Hospital is committed to excellence in serving all patients including people with disabilities.
Learn More
